If Piles (hemorrhoids) are detected at an early stage it can be treated effectively without having to do open painful surgery. Many advanced minimally invasive techniques are available like stapler ( MIPH ) and ligation (DG HAL and HAL RAR) to provide permanent solution for piles with minimal discomfort, short hospital stay and quick recovery times.
What is a hemorrhoid (piles)?
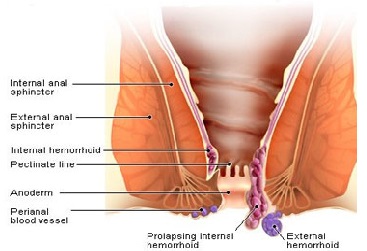
Often described as “varicose veins of the anus and rectum”, hemorrhoids are dilated and swollen cushions (pads of tissue) in the anal canal, they may project into the anal canal to form visible swellings.
There are two types, external and internal.
External hemorrhoids are near the anus and covered by skin.Internal hemorrhoids develop within the anus beneath the anal lining.
Four degrees of hemorrhoids
Hemorrhoids that bleed but do not prolapse.
Hemorrhoids that prolapse and retract on their own (with or without bleeding).
Hemorrhoids that prolapse but must be pushed back in by a finger.
Hemorrhoids that prolapse and cannot be pushed back in.
What Causes Hemorrhoids (Piles)?
Causes of piles are constipation and excessive straining during bowel movement. There are several theories, including inadequate intake of fiber, and prolonged sitting on the toilet. Pregnancy is a cause of enlarged hemorrhoids.
What are the Symptoms of Piles?
-
Bleeding during bowel movement.
-
Protrusion during bowel movement.
-
Lump
-
Pain
-
Itching and irritation
How Piles Diagnosed?
Any rectal bleeding should always be checked out by a Qualified Surgeon or Colo-rectal surgeon to rule out certain serious causes of bleeding. even if it is suspected to be from a hemorrhoid.
History of symptoms gives fair clue to diagnosis.
The diagnosis of an external hemorrhoid is easy if the hemorrhoid protrudes from the anus. For non protruding hemorrhoids rectal examination with a gloved finger is required.
Thorough examination for internal hemorrhoids is done by proctoscope and also other causes of Hemorrhoid-like symptoms can be diagnosed.
If there is rectal bleeding, the colon above the rectum needs to be examined to exclude important causes of bleeding other than piles (hemorrhoids).
Other serious causes include colorectal cancer or polyps or inflammatory bowel disease. This examination can be done by either flexible sigmoidoscopy or colonoscopy.
What is the Hemorrhoid (Piles) Treatment?
General measures (home care)
Medical Management
Preparation for procedure
Post operative what to expect?
Pre- operative preparation for anal surgery
Our Specialist

Dr. Nitish Jhawar
M.S., FMAS, FIAGES, FALS, FACRSI
Fellow Advance Laparoscopic Surgery
Fellow Colorectal Surgery USA
Senior Laparoscopic & Colorectal Surgeon
Phone No: +91 9322 229 159
Email Id: info@neoalta.com

